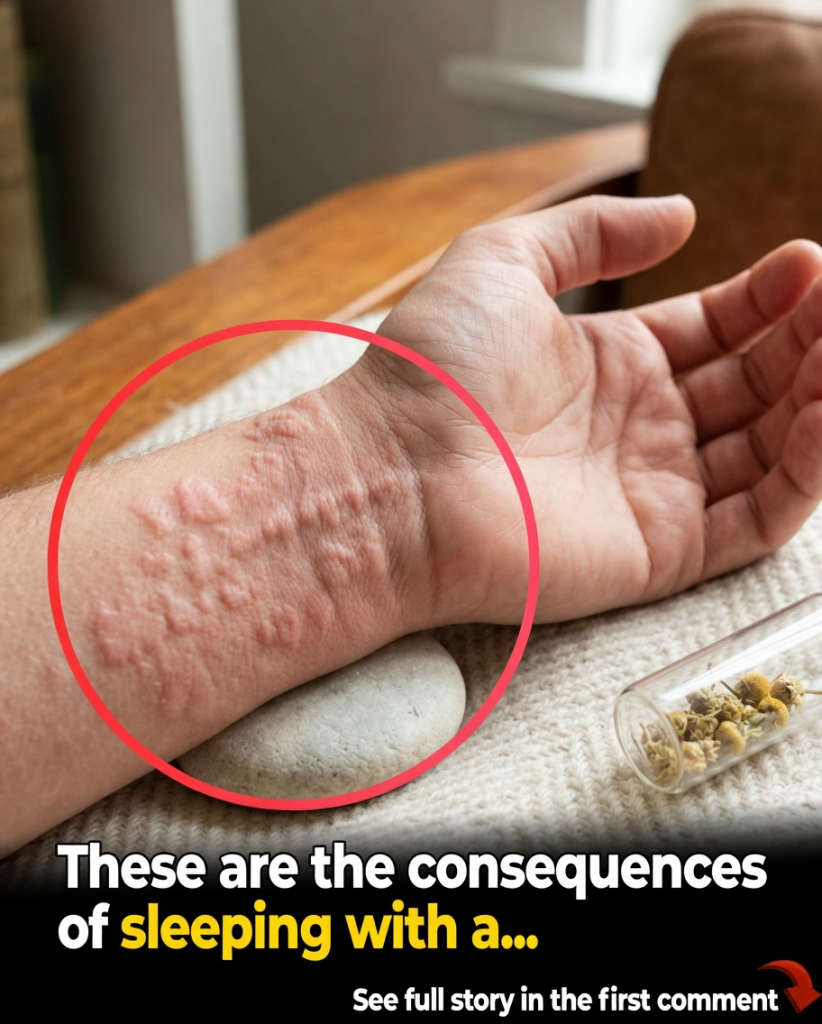
Hives can strike without warning — one minute your skin is clear, the next you’re covered in red, itchy welts that burn and sting. For some people, the outbreaks are occasional and mild. For others, they become a frustrating, recurring nightmare that disrupts sleep, work, and peace of mind. The hardest part? Many sufferers never identify the real trigger. While food allergies and stress get most of the blame, the actual causes are often far more surprising — and easier to overlook than you’d think.
Hives (medically known as urticaria) occur when your immune system releases histamine in response to a perceived threat. This causes small blood vessels to leak fluid under the skin, creating those raised, itchy bumps. They can appear anywhere on the body and usually fade within hours, only to return later. Understanding the hidden triggers is the first step toward real relief.
Here are eight common but frequently missed causes that could be behind your hives — plus practical ways to regain control.
1. Everyday Infections You’ve Already “Recovered” From
One of the most surprising triggers is a recent or lingering infection. Viral illnesses like the common cold, flu, or even a mild stomach bug can trigger hives days or weeks after the obvious symptoms disappear. Your immune system stays on high alert, overreacting to normal stimuli and flooding the skin with histamine. Bacterial infections (strep throat, sinus issues, or even dental problems) can do the same. If your hives started shortly after being sick, the infection may still be the root cause.
2. Medications You’ve Taken for Months or Years
Many people assume only new prescriptions cause reactions, but long-term medications can suddenly become problematic. Common culprits include NSAIDs (ibuprofen, naproxen), blood pressure medications, antibiotics, and even certain supplements or herbal remedies. The body’s sensitivity can change over time, turning a once-harmless pill into a hives trigger. Always review everything you take when outbreaks begin.
3. Pressure, Friction, or Tight Clothing
This is called pressure urticaria or dermographism. Simple things like tight waistbands, backpack straps, elastic, or even scratching can cause welts to appear. The reaction often shows up 30 minutes to several hours later, making the connection hard to spot. If your hives follow certain clothing patterns or appear where your skin rubs against something, pressure could be the culprit.
4. Temperature Changes (Hot or Cold)
Both heat and cold can trigger hives in sensitive people. Cold urticaria appears after exposure to cold air, cold water, or even wind chill. Heat urticaria can flare after hot showers, exercise, or warm environments. These physical triggers are often seasonal or tied to daily routines, so they’re frequently blamed on other things.
5. Exercise and Sweating
Some people develop small, intensely itchy hives during or after physical activity — a condition called cholinergic urticaria. The combination of body heat, sweat, and movement sets off the reaction. Because it happens during normal exercise, many assume it’s just “normal itching” or dry skin.
6. Sun Exposure
Solar urticaria is less common but very real. Some people break out after even brief time in the sun. The reaction can be delayed, so the connection isn’t always obvious. Sunscreen, protective clothing, and limiting peak sun hours can make a big difference.
7. Hidden Food Additives and Sensitivities
Beyond classic allergies, many people react to preservatives, artificial colors, or naturally occurring compounds like salicylates (found in many fruits and spices). These reactions can be delayed by hours or even days, making it difficult to link them to specific meals. Keeping a detailed food diary is essential for identifying these triggers.
8. Underlying Health Conditions
Chronic or recurring hives can sometimes signal bigger issues like thyroid disorders, autoimmune conditions, or infections. When standard triggers don’t explain the outbreaks, a deeper medical evaluation is often needed. Blood work and specialist input can uncover hidden causes that simple antihistamines can’t fix.
Practical Steps to Finally Get Relief
The most effective strategy is detective work combined with symptom management:
- Track everything — Use a journal or app to log food, medications, weather, stress, and activity levels.
- Start with antihistamines — Non-drowsy options like loratadine or cetirizine are usually the first line of defense.
- Simplify your environment — Switch to fragrance-free products, loose clothing, and gentle skincare.
- Manage stress — Techniques like meditation, exercise, or therapy can reduce flare frequency.
- See a specialist — An allergist or dermatologist can run tests and explore underlying causes.
Most people with hives eventually find their specific triggers and achieve significant relief. The key is patience and systematic elimination of possible causes.
Hives are frustrating and uncomfortable, but they don’t have to control your life. By looking beyond the obvious suspects and addressing the sneaky triggers hiding in your daily routine, you can finally break the cycle and enjoy clearer, calmer skin.
If you’ve been struggling with recurring hives, don’t give up on finding answers. The right combination of awareness, tracking, and professional support can make all the difference. Your skin is trying to tell you something — learning to listen is the first step toward lasting relief.
Have you discovered any unexpected triggers for your hives? Share your experience in the comments — it might help someone else finally solve their mystery.