You wake up, stretch, glance in the mirror—and freeze. Small red or purple dots have appeared on your arms, legs, or chest overnight. They don’t itch, don’t hurt, don’t look like a rash. Just tiny pinprick marks, sometimes clustered, sometimes scattered. At first you shrug it off—dry skin, maybe a new soap, or you bumped into something. But the next day there are more. And the day after that. You start Googling late at night, heart racing, because something feels wrong. You’re not alone. Thousands of people over 50 report the same thing every year, and while most cases are harmless, some are urgent red flags your body can’t afford to ignore.
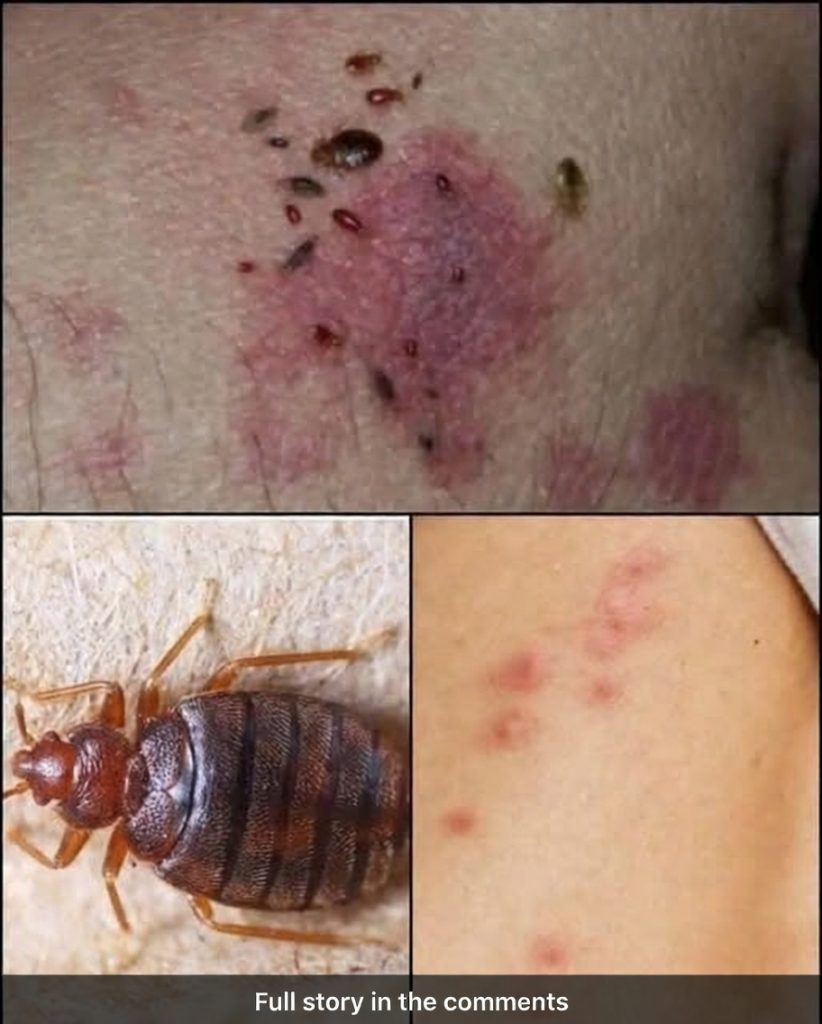
These dots are called petechiae (tiny blood spots under the skin) or purpura (slightly larger ones). They happen when small blood vessels (capillaries) break and leak red blood cells into the surrounding tissue. Unlike a regular rash that blanches (turns white) when you press on it, petechiae and purpura do not fade under pressure. That’s the first clue they’re different. They can appear suddenly after coughing hard, vomiting, heavy lifting, or even tight clothing. In those cases they usually resolve in days. But when they show up without obvious cause—especially in clusters or spreading—they can signal something far more serious happening inside.
The most common benign cause in older adults is fragile skin and blood vessels. As we age, collagen and elastin decrease, skin thins, and capillaries become more prone to rupture. Certain medications make it worse: blood thinners (aspirin, warfarin, Eliquis), steroids, NSAIDs, even some antidepressants and antibiotics. If you’re on any of these and new dots appear, call your doctor the same day. They may adjust your dose or run blood tests. But the dots that arrive without medication changes or trauma are the ones that demand attention fast.
One of the most urgent causes is low platelets (thrombocytopenia). Platelets help blood clot; when their count drops dangerously low, even minor pressure causes bleeding under the skin. Causes include viral infections, autoimmune diseases (like ITP), bone marrow problems, leukemia, or medication side effects. If petechiae appear with easy bruising, nosebleeds, bleeding gums, fatigue, or fever, go to urgent care or the ER immediately. Blood work can confirm platelet levels within hours—early detection can be lifesaving.
Another serious possibility is vasculitis—inflammation of blood vessels. Small-vessel vasculitis can cause petechiae or purpura, often on the legs, sometimes with joint pain, fever, or abdominal discomfort. It can stem from autoimmune conditions (lupus, rheumatoid arthritis), infections, or medications. Untreated, it can damage organs. A dermatologist or rheumatologist usually diagnoses it with skin biopsy and blood tests. Prompt treatment with steroids or immunosuppressants can prevent complications.
Meningococcal infection (meningitis) is the emergency most people fear. The classic “non-blanching rash” starts as petechiae that can rapidly become purpura. It spreads fast, often with fever, stiff neck, severe headache, confusion, or sensitivity to light. This is a medical emergency—call 911 immediately. Early antibiotics can be life-saving. While rare, the speed of progression makes it the one no one waits to rule out.
Liver disease and clotting disorders can also cause widespread petechiae or purpura. Cirrhosis, hepatitis, or vitamin K deficiency impair clotting factor production. Kidney problems (especially with dialysis) or certain cancers (leukemia, lymphoma) can lower platelets or damage vessels. These conditions usually come with other symptoms—jaundice, swelling, weight loss, night sweats—but skin changes can appear first.
The turning point is simple: if the dots appeared suddenly, are spreading, do not blanch when pressed, or come with any other symptom (bruising, bleeding, fatigue, fever, joint pain), see a doctor the same day or go to urgent care/ER. A simple blood test (CBC, platelet count, coagulation panel) can rule out most dangerous causes within hours. Early action prevents complications and often means simpler treatment.
Most of the time, especially in older adults, scattered petechiae are benign—medication-related, skin fragility, or minor trauma. But “most of the time” is not “always.” The cost of ignoring them can be high; the cost of checking is almost nothing. Protect your health the way you protect your family—by paying attention to small warnings.
In the reflective close, these tiny dots are your skin’s way of speaking when something inside needs help. At 50+, when Medicare covers most screenings and retirement savings are finally in place, listening to your body becomes one of the most important investments you can make. A quick doctor visit can mean peace of mind—or early treatment that saves years of worry. Don’t wait for the dots to multiply. What small change on your skin ever prompted you to see a doctor? Or what health warning do you wish you’d taken seriously sooner? Share in the comments below.