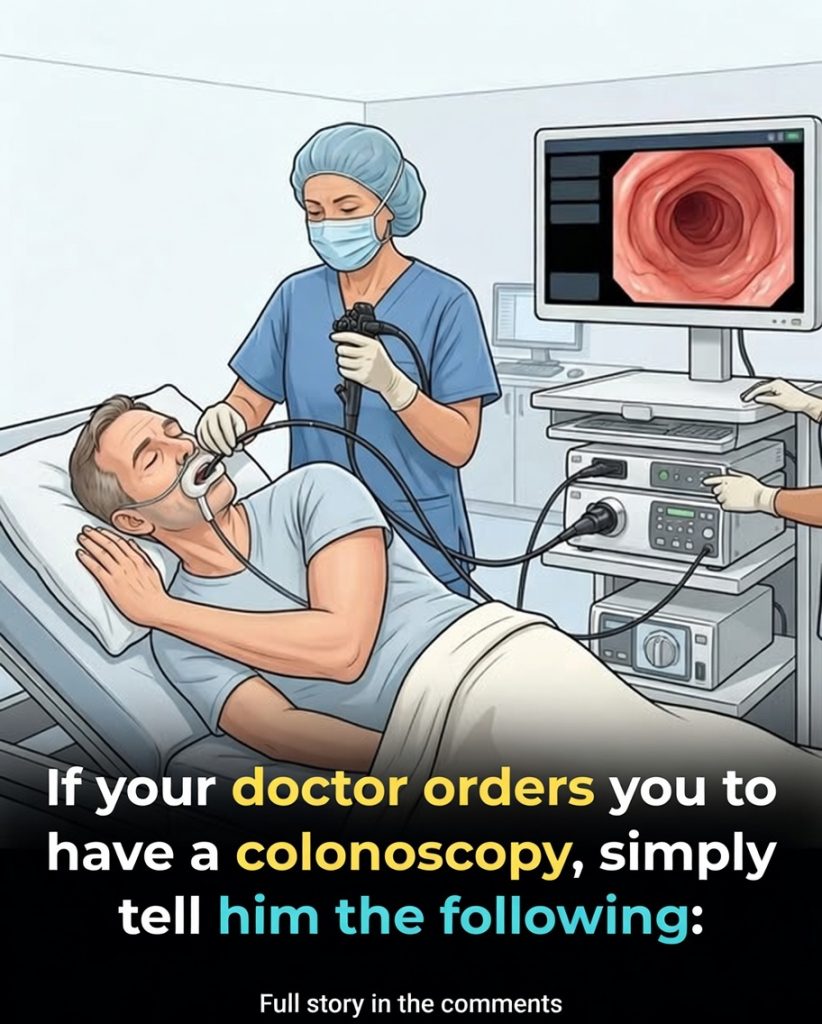
You sit in the exam room, paper gown crinkling under you, trying to focus on the doctor’s calm voice while your mind races through every embarrassing detail you’ve read online. The colonoscopy brochure lies folded on your lap, diagrams neatly labeled, but none of them capture the quiet dread that settles in your chest. At 55 you’ve reached the age where screening is no longer optional; it’s recommended, expected, lifesaving. You nod through the explanation of the prep solution, the fasting, the clear-liquid diet, the timing of the laxative doses. You understand the basics: the camera will look inside your colon to find and remove polyps before they become cancer. You know the statistics—early detection dramatically improves outcomes. Yet as the doctor finishes and asks if you have questions, one single sentence forms in your mind that most people never say out loud.
“What sedation will you use, and who will administer it?” The doctor pauses, surprised but pleased you asked. This is the question that separates routine procedures from truly safe ones. Many patients assume “sedation” means the same thing everywhere—some IV medication that makes you drowsy and forgetful. But sedation levels vary widely: moderate (conscious sedation), deep sedation, or general anesthesia. Who delivers it matters just as much. In some facilities a gastroenterologist directs a nurse to give the drugs; in others an anesthesiologist or nurse anesthetist is present throughout. The difference can mean the world if breathing slows, blood pressure drops, or you have an unexpected reaction.
You’ve already thought about your own health history: high blood pressure managed with medication, a mild sleep apnea diagnosis you use a CPAP for at night, a family history of heart issues that makes you wonder how your body will handle powerful sedatives. The doctor explains that your procedure will use moderate sedation with propofol, administered and monitored by a board-certified anesthesiologist who stays in the room the entire time. That single detail—continuous anesthesiology presence—eases the knot in your stomach more than any reassurance about polyp detection rates. You realize you almost left without asking, assuming “sedation” was standardized and safe across the board.
The complication many overlook is that not every center follows the same protocol. Some outpatient facilities use lighter sedation to cut costs and speed turnover, leaving patients more aware or requiring higher doses that increase risks. Others rely on the gastroenterologist to oversee the drugs without dedicated anesthesia support. If you have underlying conditions—sleep apnea, obesity, heart or lung issues, or even just anxiety that makes you tense—these differences can turn a routine screening into something riskier. Asking upfront lets you choose a facility that matches your needs, or at least go in knowing exactly what to expect and how your airway and vital signs will be protected.
The turning point often comes when you push for specifics. “Will an anesthesiologist be present the whole time?” “What monitoring equipment will be used—continuous pulse oximetry, capnography, blood pressure every few minutes?” “What’s the reversal plan if I have trouble breathing?” These aren’t dramatic demands; they’re practical questions that show you’re an active partner in your care. Most doctors respect the inquiry and will answer clearly. If they seem rushed or dismissive, that’s information too—perhaps time to seek a second opinion or a different center. You’re not being difficult; you’re protecting yourself at a moment when vulnerability is unavoidable.
The hidden truth is that while colonoscopy is one of the most effective cancer-prevention tools we have—removing precancerous polyps can prevent colorectal cancer entirely—the procedure’s safety hinges on preparation, monitoring, and the team in the room. The prep may be miserable, the scope itself uncomfortable even under sedation, but the real risk lies in sedation management. Asking about it empowers you to make informed choices: perhaps selecting a hospital-affiliated center over a standalone clinic, or requesting deep sedation if moderate leaves you too anxious. It also opens the door to discuss alternatives if you’re truly terrified—though for most, the standard process with proper sedation is far safer than skipping the test.
The immediate aftermath of asking feels lighter. You leave the appointment with a clear picture: anesthesiologist present, full monitoring, propofol titration tailored to your vital signs. You stock up on clear broth, sports drinks, and lemon Jell-O for the prep day. You mark the calendar, arrange a ride home, and text your adult children so they know the plan. The dread doesn’t vanish entirely—embarrassment lingers, the cleanse looms—but knowledge replaces some of the fear. You’re no longer walking blind into the unknown; you’re walking in prepared.
In the reflective close, the colonoscopy question carries a gentle, lifesaving lesson. At our age—when Medicare covers this screening with no copay, when retirement savings and home equity finally offer some security—the most powerful act isn’t bravery in the face of fear; it’s curiosity in the face of uncertainty. One simple question about sedation can shift the experience from terrifying to manageable, from risky to protected. It reminds us that advocacy for our health doesn’t end when we hand over the insurance card—it begins there. As you prep the gallon jug or sit with family discussing the appointment, ask yourself: what other small question might protect someone you love? What moment of speaking up changed a medical outcome for you or someone close? Share in the comments below.