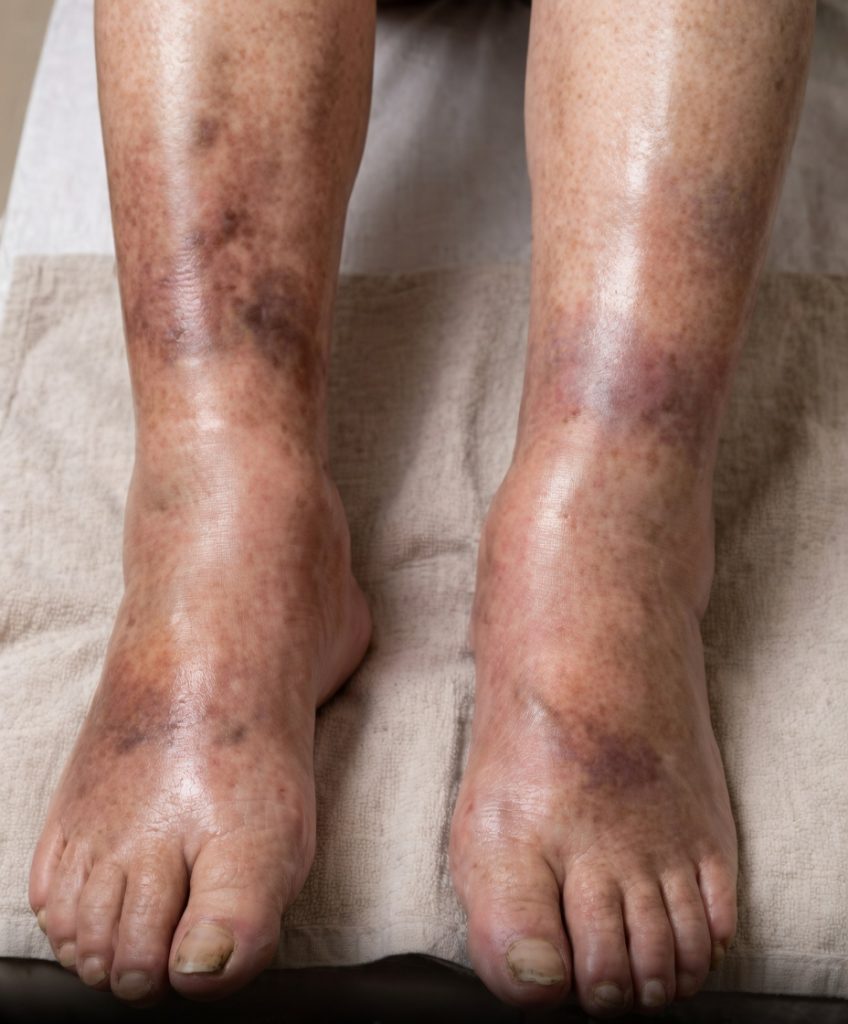
Swollen legs are so common after 40 that most people shrug them off as “normal aging,” too much standing, salty food, or just the end of a long day. Gravity pulls fluid downward, veins work harder, and mild puffiness around the ankles becomes routine. But when the swelling lingers for weeks, feels tight or painful, leaves deep sock marks, or happens even when you elevate your legs — it stops being harmless. For many, it becomes one of the earliest, quietest signals that something deeper is wrong… and the pancreas is increasingly implicated in those cases.
The pancreas sits deep in the abdomen, behind the stomach, quietly regulating blood sugar and digestion. When it becomes inflamed (pancreatitis), develops cysts, or — most seriously — harbors a tumor, it can disrupt fluid balance, blood flow, and protein levels in ways that show up first in the legs. Chronic pancreatitis or pancreatic cancer can cause low albumin (a blood protein that keeps fluid inside vessels). When albumin drops, fluid leaks into tissues — especially the lower legs and feet — creating persistent, often painless swelling called edema.
This type of swelling tends to be bilateral (both legs), pitting (leaves a dent when pressed), and resistant to usual fixes like cutting salt or elevating feet. Other clues often appear alongside it:
- Unexplained weight loss (even while eating normally)
- Dull upper abdominal or back pain that worsens after eating
- Greasy, foul-smelling stools or frequent diarrhea
- New-onset diabetes or sudden worsening of existing diabetes
- Yellowing of skin/eyes (jaundice) or dark urine
- Chronic fatigue that feels different from “just getting older”
- Loss of appetite or feeling full after small meals
These symptoms are sneaky. They creep in slowly, overlap with dozens of other conditions, and are easy to dismiss — especially when you’re busy with family, work, or retirement. But pancreatic issues progress quietly until they don’t. Early detection dramatically improves outcomes, particularly with pancreatic cancer, where survival rates drop sharply once it spreads.
What to do if swollen legs + any of these signs are present:
- See your doctor promptly — mention “persistent leg edema” and ask for basic bloodwork (albumin, liver/pancreas enzymes, fasting glucose, A1C) plus a check for deep vein thrombosis (DVT) to rule out immediate dangers.
- Request imaging if bloodwork is abnormal — abdominal ultrasound is cheap and non-invasive; CT or MRI may follow if needed.
- Track symptoms — note when swelling is worst, how it responds to elevation/salt reduction, any stool changes, appetite shifts, or new pains. Details help doctors spot patterns.
- Protect nutrition — pancreatic problems impair digestion and absorption. Focus on small, frequent meals with lean protein, healthy fats (avocado, nuts, olive oil), and cooked vegetables. Avoid heavy alcohol (a major pancreatitis trigger).
- Stay hydrated but smart — dehydration worsens edema, but too much plain water without electrolytes can dilute blood protein. Add a pinch of sea salt or eat potassium-rich foods (bananas, spinach).
For those over 50, routine checkups should already include blood sugar and liver/pancreas markers. If swelling appears suddenly or won’t budge, push for answers — don’t accept “it’s just age” as the only explanation. A simple blood test or ultrasound can rule out serious issues or catch them early when treatment works best.
This isn’t about fear — it’s about listening to your body when it whispers before it screams. Swollen legs might be nothing… but sometimes they’re the first polite knock on the door from a problem that needs attention now.
You’ve earned every year ahead. Protect them by paying attention today. If something feels off — especially with swollen legs + any of the other signs — talk to your doctor. One conversation could add years of health and peace.